Mucormycosis epidemic: another dark side to the COVID-19 pandemic
The opportunistic infection, mucormycosis, commonly called "black fungus disease" reveals another dark facet to the already devastating COVID-19 pandemic.
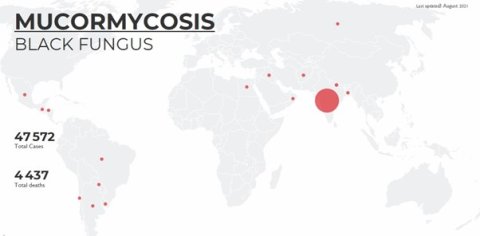
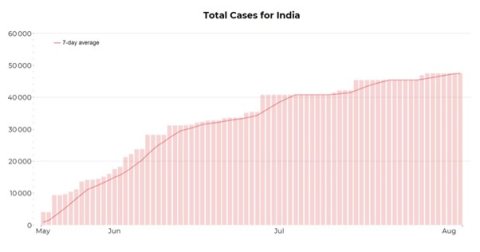
The first wave of COVID-19 in India from July to December 2020 came with an increased number of cases of mucormycosis. However, during the second wave, a huge surge of cases including a staggering 47,508 cases and 4,425 deaths due to mucormycosis have been reported from India between 5 May and 3 August 2021.
Several other countries have reported small numbers of cases during the same period. The first few cases, in the Arabian Peninsula, were reported in Oman, along with few cases in Egypt and Iraq. Many cases have also been reported in the Latin American nations of Chile and Uruguay.!
Black fungus disease
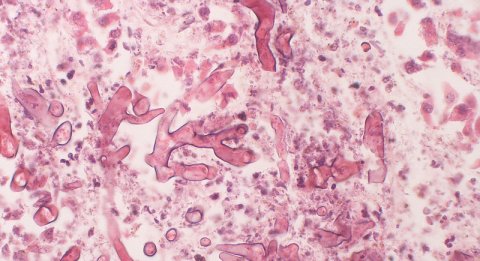
Mucormycosis is a rare opportunistic infection caused by fungi that belong to the family Mucorales and usually live in soil and decaying organic material such as vegetable matter.
Fungi that commonly cause mucormycosis include Rhizopus spp., Mucor spp., Rhizomucor spp., Cunninghamella spp, Apophysomyces spp., and Lichthemia (formerly known as Absidia) spp.
The hyphae of the causative fungus are non-pigmented. However, the older colonies become grey to brown in colour due to the development of pigmented spores. Nevertheless, the name "black fungus disease" comes from the black discolouration of the necrotic tissue that the fungus causes by invading blood vessels and destroying surrounding tissue. Mucormycosis rapidly involves neighbouring organs and can be fatal.
Who gets mucormycosis?
Although almost everyone is frequently exposed to this environmental fungus, healthy individuals do not develop the disease.
Individuals whose macrophages or neutrophils are compromised, either by function or number, are susceptible to the infection.
Hence, people with conditions such as diabetes mellitus with hyperglycemia, neutropenia, acidosis, renal failure, corticosteroid therapy, iron overload and those who are post-transplant hosts risk developing the disease.
The epidemic of mucormycosis in India
![Black necrotic area of a patient affected by mucormycosis. [Photo taken with consent of patient]](https://www.rstmh.org/sites/rstmh/files/styles/nugget-mobile/public/content/paragraphs/text/images/2021-08-18/4.jpg?itok=3RLlCpnR×tamp=1629315353)
The Indian COVID-19 associated mucormycosis (COVID-Mucor) epidemic was driven by the convergence of the following interlinked factors: uncontrolled diabetes mellitus, widespread steroid use (most of which were unwarranted), and perhaps COVID-19 itself.
The vast majority (97%) of patients with COVID-Mucor had hyperglycemia. 76% of patients with COVID-Mucor had mild COVID-19 that did not require oxygen therapy. However, steroid use was common, even in mild disease, and was strongly associated with COVID-Mucor. Additionally, there are pointers that the COVID-19 infection itself has a role to play in increasing susceptibility to mucormycosis.
Notably, after COVID-19 infection in previously euglycemic individuals, hyperglycemia that lasts up to three months, was reported. The mechanism for this is proposed to be aberrant cytokine milieu and insulin resistance. The mean serum ferritin levels, a marker of immune dysregulation and an integral part of iron metabolism, was also noted to be markedly elevated in patients with COVID-Mucor and possibly contributed to mucormycosis.
How is the infection acquired?
Mucormycosis is contracted in three ways: inhalation or ingestion of spores and contamination of wounds by spores. Inhalation and deposition of spores in the sinuses or lungs are the most common.
Types of mucormycosis
- Rhino-orbito-cerebral mucormycosis is the commonest form of the disease which starts in the sinus and slowly spreads to nearby structures including the orbital apex and the brain. This is most common in people with uncontrolled diabetes mellitus.
- Pulmonary mucormycosis is the commonest type of mucormycosis in people with cancer and those who had organ or stem cell transplant.
- Gastrointestinal mucormycosis is commoner among young children and in post-transplant hosts.
- Cutaneous mucormycosis occurs from contamination of trauma and burn wounds. This commonly occurs in immunocompetent individuals.
- Disseminated mucormycosis occurs following the spread of infection through the bloodstream. The infection then affects other parts of the body – most commonly the brain and occasionally other organs such as the spleen, heart, and skin.
Common manifestations of mucormycosis
The manifestation of mucormycosis depends on the area of involvement. The common presenting symptoms in rhino-orbito-cerebral disease are facial pain, swelling, and numbness.
Nasal block and bleeding from the nose are also noted. The initial sinusitis progresses to erode the bone. It can involve the palate resulting in a fistula, the optic nerve and other nerves at the orbital apex impairing the vision and eye movement, or the internal carotid artery through the cavernous sinus resulting in stroke and even death.
The common presenting symptoms of pulmonary mucormycosis are cough, chest pain, haemoptysis, and breathlessness. Pulmonary mucormycosis manifests as nodules, consolidation or masses on chest imaging.
The "reverse halo sign", that is an area of ground-glass opacity surrounded by a rim of consolidation is often seen on CT scans. Additionally, thick-walled cavitary lesions and pleural effusions are also seen in pulmonary mucormycosis.
Treatment of mucormycosis
The mainstay of treatment is a combination of surgical debridement and antifungal therapy after confirmation of the disease by histopathology, fungal smears and culture.
Conventional antifungal therapy includes intravenous amphotericin B for four to six weeks followed by oral treatment using posaconazole for three to six months. Further, optimal sugar control can improve the phagocytic function in these patients.
In patients with uncontrolled diabetes-related rhino-orbito-cerebral disease, the use of a shorter intravenous therapy is currently being evaluated. Posaconazole and isavuconazole are increasingly used with improved outcomes. Whereas, antifungal drugs such as fluconazole, voriconazole, and echinocandins are not effective.
Prevention of mucormycosis and its complications
As the disease is rapidly progressive, early identification is critical for an improved outcome.
Increased awareness of the disease among medical professionals and the public can help in achieving this.
Appropriate steroid use in patients with severe COVID-19 and screening and optimal control of hyperglycaemia can prevent COVID-Mucor.
Making a difference in the future
A consorted effort in increasing awareness through social media and other portals along with public engagement can have a lasting impact.
Surveillance and reporting new information and evidence are of paramount importance for increasing awareness and knowledge.
Global scientific collaboration and research on early diagnosis, improved treatment strategies, and newer antifungal agents can improve outcomes in the long-run.
References
1. Mucormycosis. https://governmentstats.com/mucormycosis/index.html. Accessed on 17 August 2021.
2. Patel A, Agarwal R, Rudramurthy SM et al Multicenter Epidemiologic Study of Coronavirus Disease-Associated Mucormycosis, India. Emerg Infect Dis. 2021 Jun 4;27(9).
3. ‘Black fungus’ detected in 3 COVID-19 patients in Oman [Internet]. [cited 2021 Aug 13]. Available from: https://www.aljazeera.com/news/2021/6/15/black-fungus-detected-covid-19-patients-oman
4. Dangerous Indian black fungus spreads to 4 more countries [Internet]. [cited 2021 Aug 13]. Available from: https://www.aa.com.tr/en/asia-pacific/dangerous-indian-black-fungus-spreads-to-4-more-countries/2264124
5. Mucormycosis. https://www.cdc.gov/fungal/diseases/mucormycosis/index.html
6. Bhanuprasad K, Manesh A, Devasagayam E et al. Risk Factors Associated with the Mucormycosis Epidemic During the COVID-19 Pandemic. Int J Infect Dis. 2021 (In press).
7. Oliver A Cornely, Ana Alastruey-Izquierdo et al. Global guideline for the diagnosis and management of mucormycosis: an initiative of the European Confederation of Medical Mycology in cooperation with the Mycoses Study Group Education and Research Consortium. Lancet Infect Dis 2019; 19: e405–21. doi: 10.1016/S1473-3099(19)30312-3.
