Skin NTDs – threat or opportunity

The title “Neglected Tropical Diseases of the Skin or Skin NTDs” is a recent designation that encompasses a group of NTDs that share a common feature, namely that they present with lesions on the surface of the body.
These include leprosy, Buruli ulcer, yaws, cutaneous and post kala-azar dermal leishmaniasis, lymphatic filariasis, onchocerciasis, mycetoma and other neglected mycoses, as well as scabies.
In setting out objectives towards control or elimination of these conditions it has proved logical to include other important conditions seen in the poorest of the world’s communities such as podoconiosis and common skin diseases under this broad umbrella. Addressing these together benefits patients, communities and health providers at national and district levels.
Early recognition

Early recognition and prompt interventions are key to achieving the key WHO milestones, as late presentation increases the risk of spread, disfigurement and disability along with social stigmatisation. While traditionally Skin NTDs have been approached as individual disease states, usually with their own dedicated programmes that address key issues from research to public health strategies, the NTD community has increasingly recognised that there is an enormous benefit to be derived from an integrated approach; this brings together strategy and operational capacity across a range of challenges posed by these diseases.
Yet it also needs to take into account the fact that progress towards WHO’s 2030 NTD roadmap may be affected by many different issues, from disease complexity to the timeline from which each was designated as a priority. This is not a race and the benefit of integration is that progress on each can benefit from advances made to reach these goals by the other disease areas.
The enormous strides made towards the elimination and alleviation of onchocerciasis and lymphatic filariasis (LF) have provided good examples for other NTDs. For instance, the widescale use of ivermectin as MDA provided early evidence of efficacy for the control of endemic scabies.
Similarly, the management of limb disability in LF has stimulated the adoption of integrated approaches which benefit other chronic lymphoedemas such as podoconiosis. Beyond this there are synergies with the plans for an integrated approach to chronic diseases; wound care for diabetic and leprosy ulcers have much in common.
A practical and integrated approach
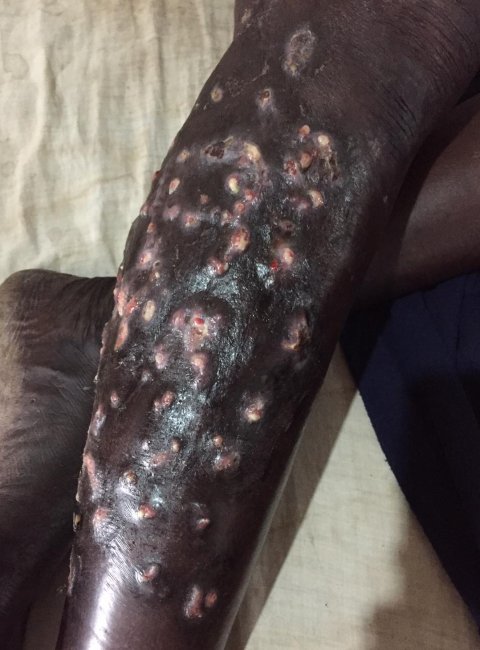
To many of us the skin is a window into what is happening in the rest of the body – including the mind.
The use of the phrase Skin NTDs to reflect a practical and integrated approach to disease recognition, disability management, social strengthening and health policy is a logical and needed initiative.
Skin NTDs are now a core part of WHO strategy and the concept has attracted support from health workers, scientists and governments.
It can only benefit that group of seemingly disparate diseases from leprosy to mycetoma that all share a common feature – they can be seen. But there is still much to be done.
Visual recognition – and discrimination between similar looking rashes – as key steps in diagnosis are not easy skills to acquire.
They partly depend on innate learning abilities that require an aptitude for the recognition of common visible patterns in different settings. Passing on these skills to other health workers is a real challenge.
Stigma and disability
Beyond diagnosis Skin NTDs are linked by common threads of stigma and disability that must be addressed. How much easier it is to do this by approaching them together.
Integration of public health strategies provide an added bonus, including maximising economies of scale. Skin NTDs also require positive actions to improve diagnosis whether this is the development of a new point of care test, a renewed focus on training in simple microbiological methods such as microscopy, or the development of clinical algorithms. There is a real opportunity here for new methods using artificial intelligence adapted to visual perception and decision making.
Lumping diseases together is sometimes seen as a threat to medical purism, but I would take the opposite view believing that this is a real opportunity to improve research and research funding, to influence the direction of public health policy and to benefit our patients and the communities in which they live.
There are signs that the funders are responding to this challenge and in the past three years some large grant calls have turned the spotlight on Skin NTDs – the first of many I hope.
In the past initially successful ventures to eliminate or control NTDs have sometimes faltered in the face of the enormity of the challenge, economic pressures, human conflict or natural disasters - and yes sometimes decisions that turned out to be wrong. Bringing these diseases together spreads the risk and provides a better classroom in which to learn.